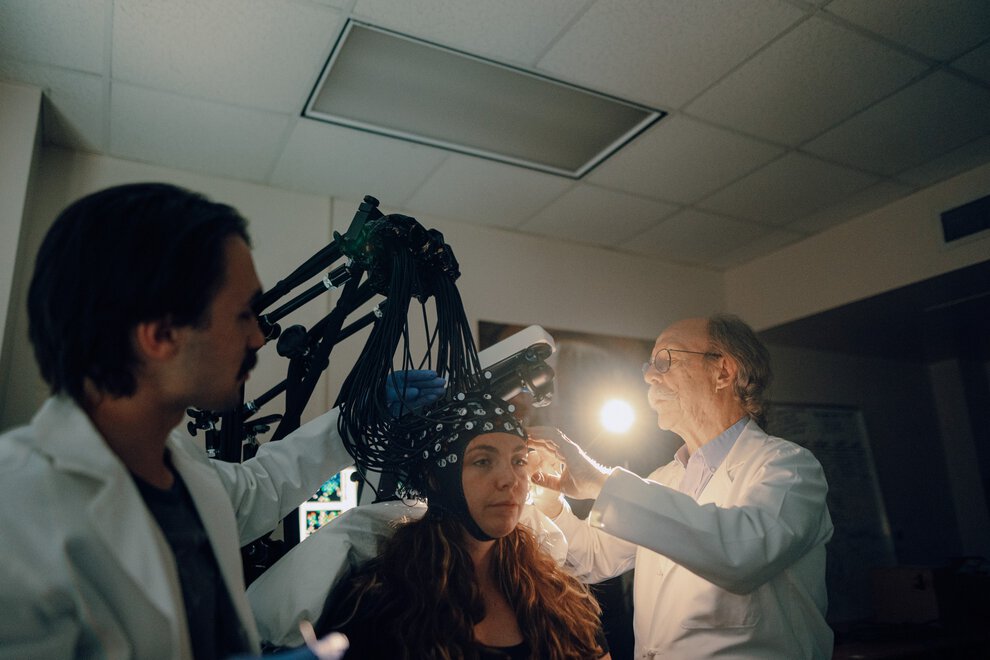
Transcranial Magnetic Stimulation (TMS)
Expert brain stimulation therapy at MUSC.
If you or a loved one is living with a hard-to-treat mental health condition like depression, OCD, or nicotine dependence, you may benefit from Transcranial Magnetic Stimulation (TMS)—a non-invasive, FDA-approved treatment offered by the expert Brain Stimulation team at the MUSC Institute of Psychiatry. This treatment works through neuromodulation – the stimulation and alteration of nerves that research has shown are involved in mood and behavior.
MUSC Health offers three options for TMS, personalized to your needs: Repetitive TMS (rTMS), Accelerated TMS, and SNT TMS (formerly known as SAINT TMS). We are the first in South Carolina to offer rTMS for OCD and nicotine dependence, and the first on the East Coast to provide SNT TMS for depression—an innovative approach with a nearly 80% remission rate. Our team is here to help you explore your options and find new hope, even when other treatments haven’t been successful.
Additional brain stimulation therapies we offer.
TMS offers new hope
Our Locations
MUSC offers brain stimulation therapy at these locations.
MUSC Health Brain Stimulation Clinic - Coleman Blvd
- Monday8 a.m. to 5 p.m.
- Tuesday8 a.m. to 5 p.m.
- Wednesday8 a.m. to 5 p.m.
- Thursday8 a.m. to 5 p.m.
- Friday8 a.m. to 5 p.m.
- SaturdayClosed
- SundayClosed
- Brain Stimulation
- Psychiatry
MUSC Health Brain Stimulation Clinic at Institute of Psychiatry
67 President Street
5th Floor
Charleston, SC 29425 Get Directions
- Monday8 a.m. to 5 p.m.
- Tuesday8 a.m. to 5 p.m.
- Wednesday8 a.m. to 5 p.m.
- Thursday8 a.m. to 5 p.m.
- Friday8 a.m. to 5 p.m.
- SaturdayClosed
- SundayClosed
- Brain Stimulation
- Psychiatry
Learn more about TMS at MUSC Health
MUSC Health offers all variations of TMS to treat depression, OCD, and support smoking cessation. During treatment, patients relax while a small device delivers targeted MRI-strength magnetic pulses to the areas of the brain involved in mood regulation.
Approximately 30% of patients with severe depression fail to respond to treatment with antidepressants. Before TMS was available, these treatment-resistant patients often received Electroconvulsive Therapy (ECT). While ECT can be highly effective, some patients experience unwanted side effects, including short-term memory loss or headaches. ECT treatments require patients to take time off work and avoid driving, making it impractical for many individuals.
TMS offers more convenience and provides good outcomes for patients who have treatment-resistant depression. Accelerated TMS can be especially beneficial for individuals who have not found relief from depression through conventional treatments. It offers new hope and a chance for a better quality of life.
Obsessive compulsive disorder (OCD) is a chronic, often disabling disorder defined by distressing and intrusive thoughts and repetitive behaviors that the person feels driven to do. About 40% of people with OCD do not respond to medications or OCD therapy, and few people find their symptoms resolved.
TMS was FDA-approved in 2018 for the treatment of OCD. By activating the neurocircuitry of OCD and then stimulating those regions, TMS can reduce symptoms in people with treatment resistance to medications and OCD therapy. According to the FDA, 38% of patients receiving TMS had at least a 30% reduction in symptoms. Recent real-world data has proven TMS to be even more successful for OCD treatment than originally thought, with nearly 58% of patients receiving a clinically significant response to treating OCD symptoms. Studies show that TMS works differently from traditional OCD medications and therapy, so even if those treatments haven’t helped, TMS still might.
MUSC Health was the first health system in South Carolina to offer TMS treatment for OCD.
Smoking is one of the leading causes of death in developed countries. The addiction to nicotine, similar to the addiction to drugs and alcohol, involves modulation of the brain reward system and causes the uncontrollable desire to smoke. Cigarette smoking has been found to harm nearly every organ system in the body and is the leading cause of preventable death in the U.S. and of disease burden worldwide. Many people can't quit alone and fail to respond to nicotine replacement therapies.
TMS was FDA-approved for smoking cessation in 2020. It works by targeting areas of the brain linked to cravings, helping reduce the urge to smoke. In a clinical trial, people who completed the treatment were more than twice as likely to quit smoking compared to those who received a placebo—and even those who didn’t quit smoked fewer cigarettes each day.
MUSC Health was the first health system in South Carolina to offer TMS treatment for smoking cessation.
As a patient at the MUSC Health Department of Psychiatry, Brain Stimulation Division, you will receive bills from the physicians and from the hospital. MUSC Physicians (MUSCP) submits bills for the professional fees charged by its physicians. The Medical University Hospital Authority (MUHA) bills for hospital facility charges covering the use of equipment, space, and supplies. Both MUSC entities participate with Medicare, BlueCross BlueShield, and various other payers and managed care organizations. They do not, however, participate with all payers. Regulations also require us to bill for deductibles and co-payments, even for those insurances with which we participate. Co-payments will be required before or at the time of service.
MUHA may participate with a health plan, but MUSCP may not. In this instance, you would be responsible for paying for the portion of your physician's bill that your insurance plan does not cover. Depending upon your insurance, you may not receive a bill at all, but instead receive an explanation of benefits, which will outline what your insurance was charged and what was paid on your behalf.
In some instances, your insurance requires a prior authorization before you begin treatment. Without the prior authorization, you will be required to pay for all bills. Some insurers do not require a prior authorization, but whether an authorization is required, it's still not a guarantee of payment. All payments are based on medical necessity and cannot be determined until the claim is processed. The medical documentation will be reviewed in order for the insurance company to determine payment. Thus, there is no guarantee how much is covered and if the insurance company does not cover, then the patient is responsible for payment.
Although the FDA approved TMS for the treatment of major depressive disorder in 2008, currently not all insurers are willing to cover TMS for treatment-resistant depression. TMS has evidence to treat depression after 1 medication treatment failure, but some insurers will not cover TMS unless a patient has failed to respond to 4 antidepressant medications of adequate duration and dose during this depressive episode and a trial of psychotherapy. Generally, insurers will not cover TMS for depression in patients with a diagnosis of bipolar disorder.
Disclaimer
Rates and discounts do change, be sure to confirm with the Brain Stimulation Service for any changes in charges that may not have been updated on this website.
Making lives better. Every day.
Frequently Asked Questions about TMS
Repetitive Transcranial Magnetic Stimulation (rTMS) involves applies magnetic pulses that can induce electrical currents in focused areas within the brain. The frequency (how fast or slow) of pulses activate or inhibit brain cells. High frequency rTMS in prefrontal brain regions stimulate neurons involved in mood regulation. rTMS may modify brain circuits, neuron growth factors (BDNF), neurotransmitters (serotonin, dopamine), and increase brain-derived (endogenous) opioids.
rTMS was initially a tool for neuroscience investigation of the brain. It has subsequently been studied and FDA approved for depression at this time. It is under investigation for other neuropsychiatric and pain disorders, but not FDA approved. Some insurers do cover rTMS for the treatment of unipolar depression, not other neuropsychiatric conditions. Antidepressant medications and psychotherapy are the first line treatments for major depression, but don’t work for a third of patients. rTMS is used as next-level treatment and may augment antidepressant medications or psychotherapy. Patients who have failed to achieve an adequate response from antidepressants, psychotherapy, or who are unable to tolerate medications, might consider rTMS therapy.
A patient sits in a treatment chair. Patients are asked to remove any magnetic-sensitive objects (such as jewelry) since rTMS uses magnetic pulses that can heat magnetic metals. Patients wear earplugs during treatment for hearing protection, as rTMS produces a loud clicking sound with each pulse.
During the first session, a motor threshold is found. This is the amount of machine energy needed to make the hand move when the coil is placed on the head in areas associated with movement. This measure tells the physician the patient’s rTMS treatment dose to stimulate neurons. The rTMS coil is properly positioned over the patient’s head for the motor threshold and subsequently repositioned into the treatment location. During the treatment, the patient hears a series of clicking sounds and feels a tapping sensation on their head under the treatment coil.
The treatment sensation can be initially uncomfortable. Thus we use lower doses for the first 3 sessions to help the patient accommodate to the treatment. Commonly the patient’s sensation modifies and while the stimulation is still felt, it is no longer uncomfortable.
rTMS is always prescribed by a rTMS physician and then administered by a rTMS operator. A motor threshold is always determined by a rTMS physician. The treatment itself is administered by an experienced rTMS operator under the supervision of the rTMS physician or by the rTMS physician themselves.
The rTMS operator or physician will always be present to monitor the patient during the treatment. The patient can stop a treatment at any time by verbalizing this request to the rTMS operator.
It depends on the rTMS protocol and machine type. Some conventional, FDA-approved rTMS protocols can take upwards to an hour, but generally take about 30 minutes. Other protocols can be done in 20 minutes or less. The success of the treatment is dependent not on a single session but a series of sessions that are commonly done 5 days a week for 4 to 6 weeks followed by a 3 week taper. We commonly taper by giving 3 treatments in week 1 taper, 2 treatments in week 2 taper, and 1 treatment in week 3 taper.
No. Unlike ECT, rTMS does not require any sedation or general anesthesia, so patients are fully awake and aware during the treatment. There is no “recovery time”, so patients can drive home afterwards and return to their usual activities. This also means that rTMS is not offered during hospitalization either. Future research is needed to show that rTMS can be done effectively in an inpatient setting and reduce hospitalization duration, improve outcomes, and reduce rehospitalization rates before insurers will agree to pay for inpatient rTMS.
There are few side effects associated with rTMS. Pain sensation at the site stimulation is common early in the rTMS series. This significantly decreases over the course of rTMS stimulation. Thereafter the most common side effect is headache, which is reported in nearly half of patients treated with rTMS. Headaches are mild and generally diminish over the course of the treatment. Over-the-counter pain medication, such as ibuprofen, can be used to treat these headaches.
The rTMS machine produces a loud noise. No evidence suggests there is hearing loss if earplugs are worn during the treatment.
rTMS is not associated with many of the side effects caused by medications, such as gastrointestinal upset, dry mouth, sexual dysfunction, weight gain, or sedation.
The most serious but rare risk of rTMS is seizures. However, the risk of a seizure is exceedingly low. We have never had a patient have a seizure from rTMS at MUSC Health.
Patients with any type of non-removable metal in their heads (not including braces or dental fillings) should not receive rTMS. rTMS in those situations could cause objects to heat up, malfunction, and result in serious injury or death. Below is a list of metal implants that can prevent a patient from receiving rTMS:
- Aneurysm clips or coils
- Stents in the neck or brain
- Implanted stimulators
- Electrodes to monitor brain activity
- Metallic implants in your ears and eyes
- Shrapnel or bullet fragments in or near the head
- Facial tattoos with metallic or magnetic-sensitive ink
- Other metal devices or object implanted in or near the head
Please ask a rTMS physician if you would be excluded from rTMS based on one of these conditions above.
Before scheduling you for rTMS treatment, you must first be evaluated by one of our rTMS psychiatrists to determine if rTMS would be safe and appropriate for you. If you are requesting insurance to cover the rTMS therapy, then the clinic service will seek insurance authorization, which commonly takes days to weeks for confirmation.
While there are other rTMS clinics in South Carolina, MUSC Health currently has 2 rTMS clinics in the Charleston area. One clinic is downtown at the Institute of Psychiatry, 67 President Street, near our research lab and ECT suite. The other clinic is in Mount Pleasant at 1280 Hospital Drive, Suite 200.









