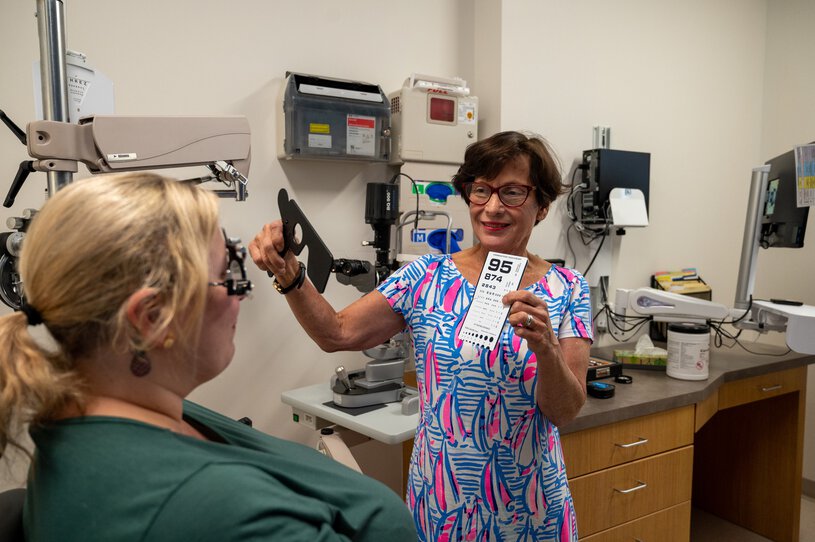
Cataract Surgery
State-of-the-art expertise in cataract surgery.
Getting older does not have to mean your vision will worsen. If you are suffering from the effects of cataracts, our experts can help. We offer the complete range of treatments, including laser-assisted surgery and eye surgery for lens replacement. We also treat other, less common causes of cataracts, including rare cases in children.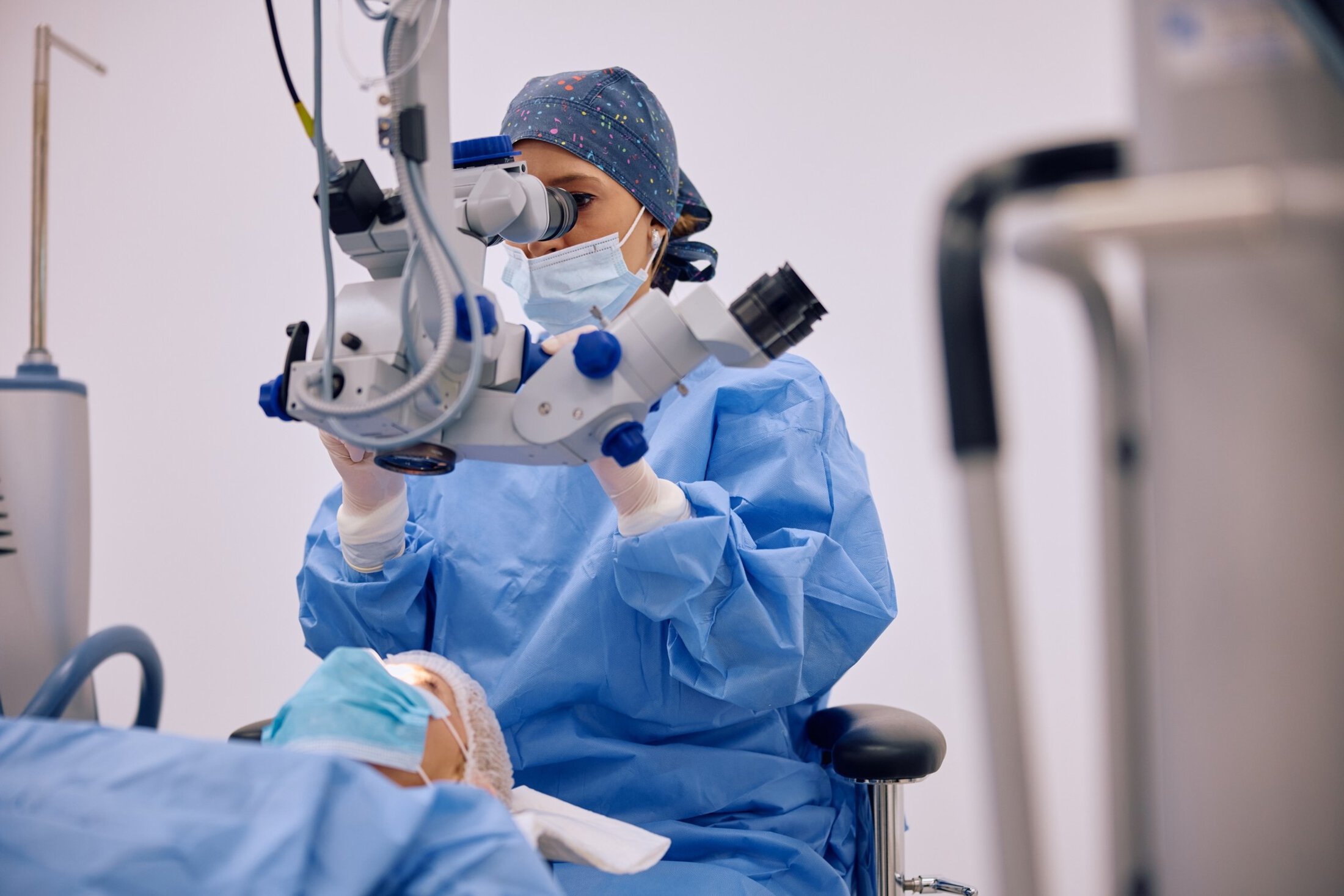
What are cataracts?
A cataract develops when your eye lens becomes cloudy, in a process called opacification. A cataract develops when the lens becomes cloudy. You may have a cataract in one or both eyes. The condition is a natural part of aging and is common among people in their late 60s and 70s. Cataracts can occasionally develop before then for other reasons, including in children.
Lens clouding may progress to the point that once-simple tasks such as reading and driving at night become difficult. Cataract surgery is typically all it takes to restore your vision. We offer all the latest cataract surgery options so you receive care that’s right for you.
Cataract Statistics
What are common symptoms of cataracts?
You may be suffering from cataracts if you're experiencing any of the following symptoms:
- Blurry vision or cloudy vision
- Double vision
- Difficulty seeing clearly while conducting daily tasks
- Light sensitivity
- Difficultly seeing clearly at night
- Dulled or faded colors
- More frequent changes to eyeglass or contact lens prescriptions
- Seeing halos around light sources
Consult your physician if you believe you're experiencing any of these symptoms.
Cataract surgical locations.
MUSC Health Ophthalmology Camden
Camden, SC 29020
- Monday8:30 a.m. to 5 p.m.
- Tuesday8:30 a.m. to 5 p.m.
- Wednesday8:30 a.m. to 5 p.m.
- Thursday8:30 a.m. to 5 p.m.
- Friday8:30 a.m. to 5 p.m.
- SaturdayClosed
- SundayClosed
- Ophthalmology
MUSC Health Glaucoma Surgery
1101 Waterline Street
Clements Ferry Pavilion, 3rd Floor
Charleston, SC 29492
- Monday8 a.m. to 5 p.m.
- Tuesday8 a.m. to 5 p.m.
- Wednesday8 a.m. to 5 p.m.
- Thursday8 a.m. to 5 p.m.
- Friday8 a.m. to 5 p.m.
- SaturdayClosed
- SundayClosed
- Ophthalmology
MUSC Health Cataract & Cornea Surgery
1101 Waterline Street
Clements Ferry Pavilion, 3rd Floor
Charleston, SC 29492
- Monday8 a.m. to 5 p.m.
- Tuesday8 a.m. to 5 p.m.
- Wednesday8 a.m. to 5 p.m.
- Thursday8 a.m. to 5 p.m.
- Friday8 a.m. to 5 p.m.
- SaturdayClosed
- SundayClosed
- Ophthalmology
Cataract surgery at Storm Eye Institute.
MUSC Health Storm Eye Institute delivers complete care for cataracts, including an accurate diagnosis and a broad range of treatment options. Our team includes eye surgeons who perform cataract surgery every week, a level of experience that helps you get the best possible care.
Highlights of our program include:
Latest Technology: We offer the best available technologies, including the femtosecond laser. This tool helps us perform surgery with a high level of precision.
Coordinated Care for Multiple Eye Conditions: It’s common to have both a cataract and another eye condition such as glaucoma at the same time. At MUSC Health, you can potentially get relief from both through one procedure. Find out more about our care for glaucoma.
Pediatric Expertise: MUSC Health is home to the only pediatric ophthalmologist in South Carolina specializing in pediatric cataract surgery. This level of expertise leads doctors from across the state to refer children to our program. Find out more about our pediatric ophthalmology.
If vision problems from cataracts are preventing you from going about your daily life, it’s important to get treatment. As a progressive eye disease, cataracts become worse over time and may lead to blindness. Our team of expert cataract surgeons will help you achieve clear vision, possibly without the need of glasses.
Cataract surgery is performed by replacing the natural lens of the eye with one called an intraocular lens, also known as an IOL. A cataract surgeon will help determine the right IOL for you from the following selections:
- Monofocal Lenses: This lens is good for distance vision, meaning it helps you see objects that are far away. You will still need to wear glasses to see objects up close, such as when you’re reading. Monofocal IOLs are usually covered by insurance.
- Accommodative Lenses: This lens changes shape when necessary, allowing your eyes to maintain focus at different distances. Accommodative IOLs are not covered by insurance.
- Multifocal Lenses: Similar to bifocal glasses, multifocal lenses have two zones set at different magnifying powers: one for distance and one for near vision. With multifocal lenses, you may only need to wear glasses if you are reading small print. Multifocal lenses are not covered by insurance.
- Toric Lenses: If you have an uneven curve on the front surface of the eye (astigmatism), a toric lens can correct it so you won’t need to wear glasses. Toric lenses are not covered by insurance.
Laser assisted cataract surgery is gentler on your eyes and may lower your risk of complications like eye infections. Eye surgeons at the Storm Eye Institute use the CATALYS Femtosecond Precision Laser System to replace the eye’s cloudy lens with a clear new artificial one. With precision-based laser assisted eye surgery, there is a shorter recovery time, meaning you can return to your daily activities soon-after. This service is not currently covered by insurance.
Our comprehensive approach means we do everything possible to help you have clear vision. You may be eligible to receive additional treatments, including:
Glaucoma Surgery: Our glaucoma treatments include laser assisted and minimally invasive procedures. Find out more about glaucoma.
YAG Laser Treatment: After cataract surgery, the protective lining that holds the IOL in place may develop a hazy film. We use the YAG laser to remove the film so you can once again see clearly.
Frequently Asked Questions About Cataracts
Cataract surgery is performed by an Ophthalmologist in under an hour (usually 10-15 minutes).
Most patients recover very quickly and can return to their daily activities within a few days.
The possible risks associated with cataract surgery include: pain and redness, swelling, floaters or changes in vision. These complications are very rare.
Cataract surgery is not painful but you might experience some mild discomfort. The physician will numb your eye with anesthetic eye drops so that you do not feel anything during the procedure.